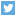A Broviac®/Hickman® central venous line (CVL) is a special intravenous (IV) line inserted under the skin on the chest wall and into a large vein that leads to the heart. It’s used in children and teens who need IV therapy for a long time.
Below you will find a variety of resources to help you better understand, cope with and/or support someone with a broviac central line.
| Fact sheets |
|
You are free to copy and redistribute these materials in any medium or format. This work may not be used for commercial purposes. View the full Creative Commons license. |
Disclaimer
These resources are for educational purposes only. If you have any questions, ask your health-care provider.